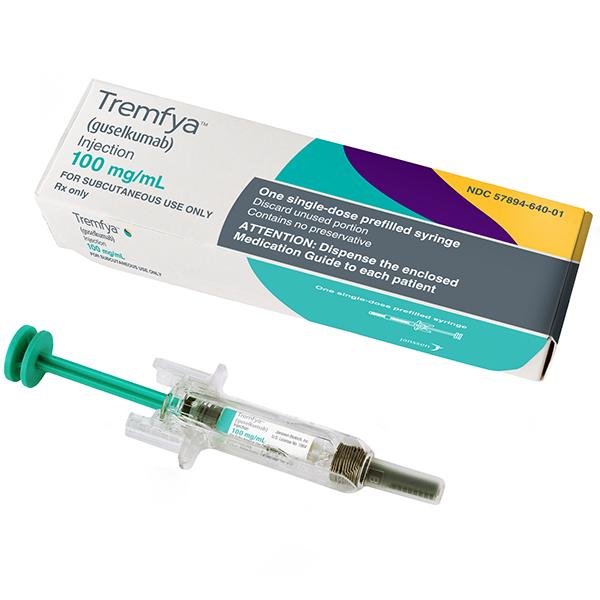
Guselkumab Injection
Function and indication: ThisFunction and indication: This product is suitable for adult patients with moderate to severe plaque psoriasis who are suitable for systemic treatment. Dosage and administration: This product should be used under the guidance and supervision of a physician who should have experience in the diagnosis and treatment of plaque psoriasis. The recommended dose of this product is 100 mg subcutaneously at week 0 and week 4, and then maintained at the same dose every 8 weeks. Patients who have not responded after 16 weeks of treatment should consider stopping the drug. Renal/liver impairment This product has not been studied in these patient groups. Therefore, a recommended dose cannot be provided. Administration method Subcutaneous administration. Injection in skin areas with psoriasis symptoms should be avoided as much as possible. After appropriate training in subcutaneous injection techniques, patients can inject this product themselves if the physician deems it appropriate. However, the physician should still ensure appropriate medical follow-up of the patient. Patients should be instructed to inject the full dose of this product according to the “Guide to Use” provided in the carton. Adverse reactions: Safety characteristics summary The most common adverse drug reaction (ADR) is upper respiratory tract infection. Adverse reactions list Table 1 lists adverse drug reactions reported in clinical studies and post-marketing experience in psoriasis. Adverse reactions are classified by MedDRA system organ class and frequency using the following rules: very common (≥1/10), common (≥1/100 to <1/10), uncommon (≥1/1,000 to <1/100), rare (≥1/10,000 to <1/1,000), very rare (<1/10,000), unknown (cannot be estimated from available data). Table 1: List of adverse reactions System organ class Frequency ADR Infections and infestations Very common Respiratory tract infections Occasionally Gastroenteritis Occasionally Herpes simplex infections Occasionally Ringworm infections Various investigations Common Transaminases elevated Occasionally Neutrophil count decreased Immune system disorders Occasionally Hypersensitivity reactions Occasionally Allergic reactions Nervous system disorders Common Headache Gastrointestinal disorders Common Diarrhea Skin and subcutaneous tissue disorders Occasionally Urticaria Occasionally Rash Various Musculoskeletal and connective tissue disorders Common Arthralgia Systemic disorders and administration site reactions Common Injection site erythema Common Infusion site reactions Occasionally Injection site pain Description of specific adverse reactions Gastroenteritis During the placebo-controlled period of two Phase III clinical studies, the incidence of gastroenteritis was higher in the guselkumab-treated group (1.1%) than in the placebo-treated group (0.7%). Gastroenteritis was reported in 4.9% of subjects treated with guselkumab through Week 156. Adverse reactions Gastroenteritis was a non-serious event that did not lead to discontinuation of guselkumab through Week 156. Injection Site Reactions Two Phase III clinical studies lasting up to 48 weeks showed that injection site reactions occurred in 0.7% of guselkumab injections and 0.3% of placebo injections. By Week 156, injection site reactions occurred in 0.5% of guselkumab injections. Adverse Reactions Injection site erythema and injection site pain were generally mild to moderate in severity, with no serious adverse reactions; none led to discontinuation of guselkumab. Immunogenicity The immunogenicity of guselkumab was assessed using sensitive and resistant immunoassays. Based on a pooled analysis of Phase II and Phase III studies, anti-drug antibodies developed in <6% of patients treated with guselkumab over a treatment period of up to 52 weeks. Of the subjects who developed anti-drug antibodies, approximately 7% had antibodies that were classified as neutralizing, equivalent to 0.4% of all patients treated with guselkumab. Based on a pooled analysis of Phase III studies, anti-drug antibodies developed in approximately 9% of patients treated with guselkumab over a treatment period of up to 156 weeks. Anti-drug antibodies were not associated with reduced efficacy or injection site reactions. Contraindications: Severe hypersensitivity to the active ingredient or any of the listed excipients is contraindicated. •Contraindicated in patients with clinically significant active infections (e.g., active tuberculosis). •Contraindicated in combination with other drugs due to lack of compatibility studies product is suitable for adult patients with moderate to severe plaque psoriasis who are suitable for systemic treatment. Dosage and administration: This product should be used under the guidance and supervision of a physician who should have experience in the diagnosis and treatment of plaque psoriasis. The recommended dose of this product is 100 mg subcutaneously at week 0 and week 4, and then maintained at the same dose every 8 weeks. Patients who have not responded after 16 weeks of treatment should consider stopping the drug. Renal/liver impairment This product has not been studied in these patient groups. Therefore, a recommended dose cannot be provided. Administration method Subcutaneous administration. Injection in skin areas with psoriasis symptoms should be avoided as much as possible. After appropriate training in subcutaneous injection techniques, patients can inject this product themselves if the physician deems it appropriate. However, the physician should still ensure appropriate medical follow-up of the patient. Patients should be instructed to inject the full dose of this product according to the "Guide to Use" provided in the carton. Adverse reactions: Safety characteristics summary The most common adverse drug reaction (ADR) is upper respiratory tract infection. Adverse reactions list Table 1 lists adverse drug reactions reported in clinical studies and post-marketing experience in psoriasis. Adverse reactions are classified by MedDRA system organ class and frequency using the following rules: very common (≥1/10), common (≥1/100 to <1/10), uncommon (≥1/1,000 to <1/100), rare (≥1/10,000 to <1/1,000), very rare (<1/10,000), unknown (cannot be estimated from available data). Table 1: List of adverse reactions System organ class Frequency ADR Infections and infestations Very common Respiratory tract infections Occasionally Gastroenteritis Occasionally Herpes simplex infections Occasionally Ringworm infections Various investigations Common Transaminases elevated Occasionally Neutrophil count decreased Immune system disorders Occasionally Hypersensitivity reactions Occasionally Allergic reactions Nervous system disorders Common Headache Gastrointestinal disorders Common Diarrhea Skin and subcutaneous tissue disorders Occasionally Urticaria Occasionally Rash Various Musculoskeletal and connective tissue disorders Common Arthralgia Systemic disorders and administration site reactions Common Injection site erythema Common Infusion site reactions Occasionally Injection site pain Description of specific adverse reactions Gastroenteritis During the placebo-controlled period of two Phase III clinical studies, the incidence of gastroenteritis was higher in the guselkumab-treated group (1.1%) than in the placebo-treated group (0.7%). Gastroenteritis was reported in 4.9% of subjects treated with guselkumab through Week 156. Adverse reactions Gastroenteritis was a non-serious event that did not lead to discontinuation of guselkumab through Week 156. Injection Site Reactions Two Phase III clinical studies lasting up to 48 weeks showed that injection site reactions occurred in 0.7% of guselkumab injections and 0.3% of placebo injections. By Week 156, injection site reactions occurred in 0.5% of guselkumab injections. Adverse Reactions Injection site erythema and injection site pain were generally mild to moderate in severity, with no serious adverse reactions; none led to discontinuation of guselkumab. Immunogenicity The immunogenicity of guselkumab was assessed using sensitive and resistant immunoassays. Based on a pooled analysis of Phase II and Phase III studies, anti-drug antibodies developed in <6% of patients treated with guselkumab over a treatment period of up to 52 weeks. Of the subjects who developed anti-drug antibodies, approximately 7% had antibodies that were classified as neutralizing, equivalent to 0.4% of all patients treated with guselkumab. Based on a pooled analysis of Phase III studies, anti-drug antibodies developed in approximately 9% of patients treated with guselkumab over a treatment period of up to 156 weeks. Anti-drug antibodies were not associated with reduced efficacy or injection site reactions. Contraindications: Severe hypersensitivity to the active ingredient or any of the listed excipients is contraindicated. •Contraindicated in patients with clinically significant active infections (e.g., active tuberculosis). •Contraindicated in combination with other drugs due to lack of compatibility studies
Share:
Products
Our offers
Health Classification
Let us work together to protect precious health